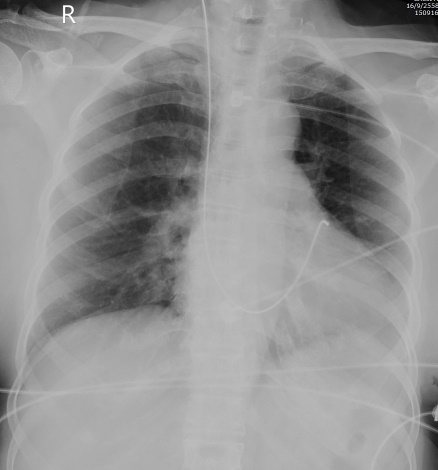
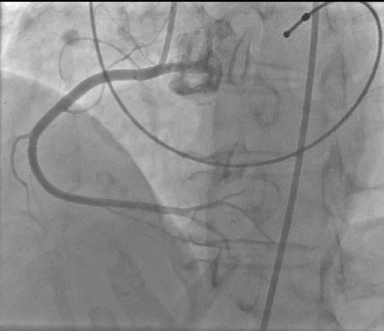
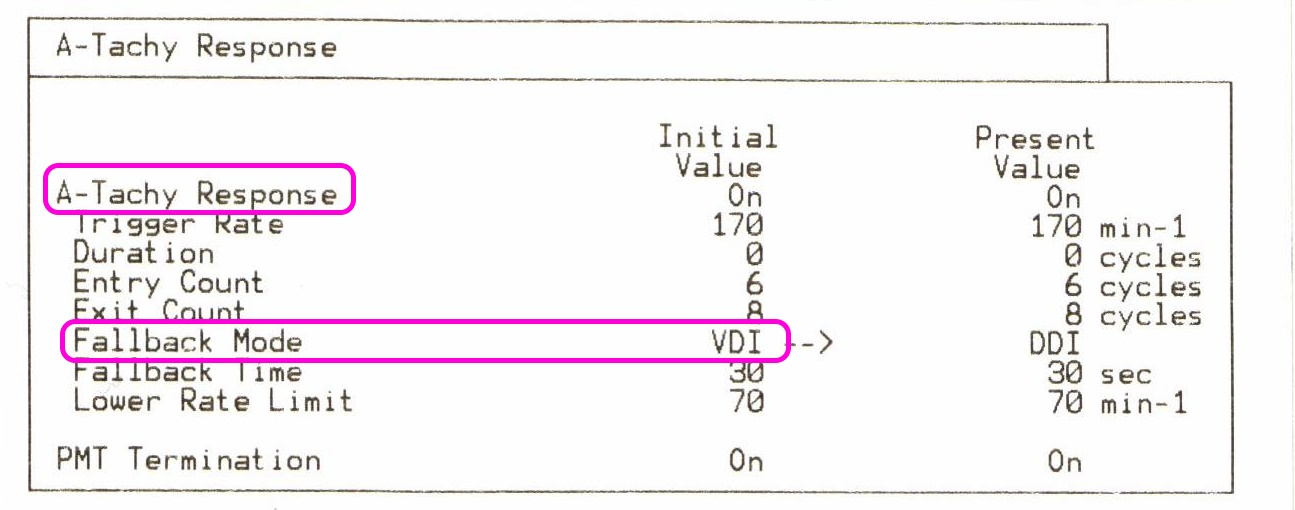
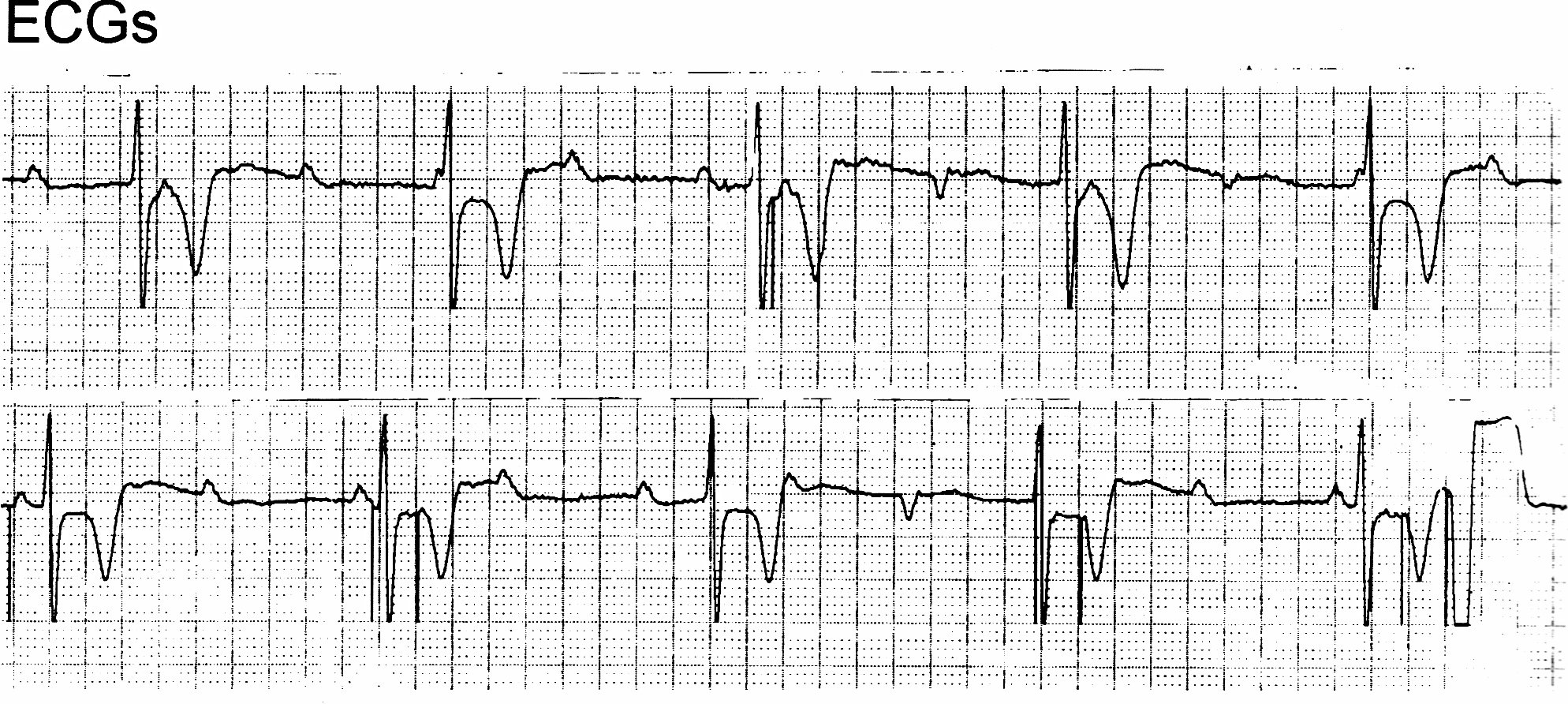
Cardiac Rhythm Device Troubleshooting
 1
1
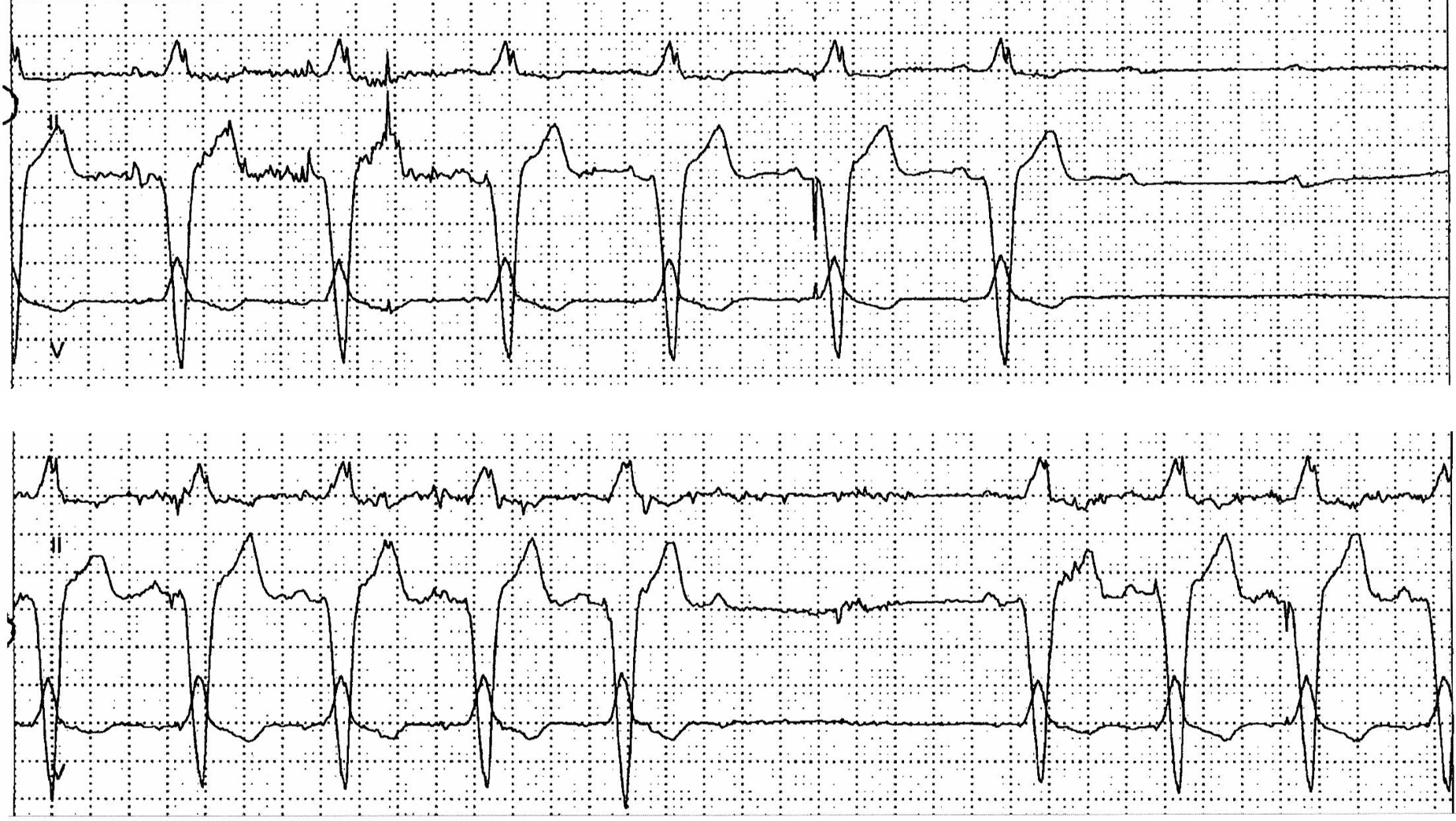 2
2
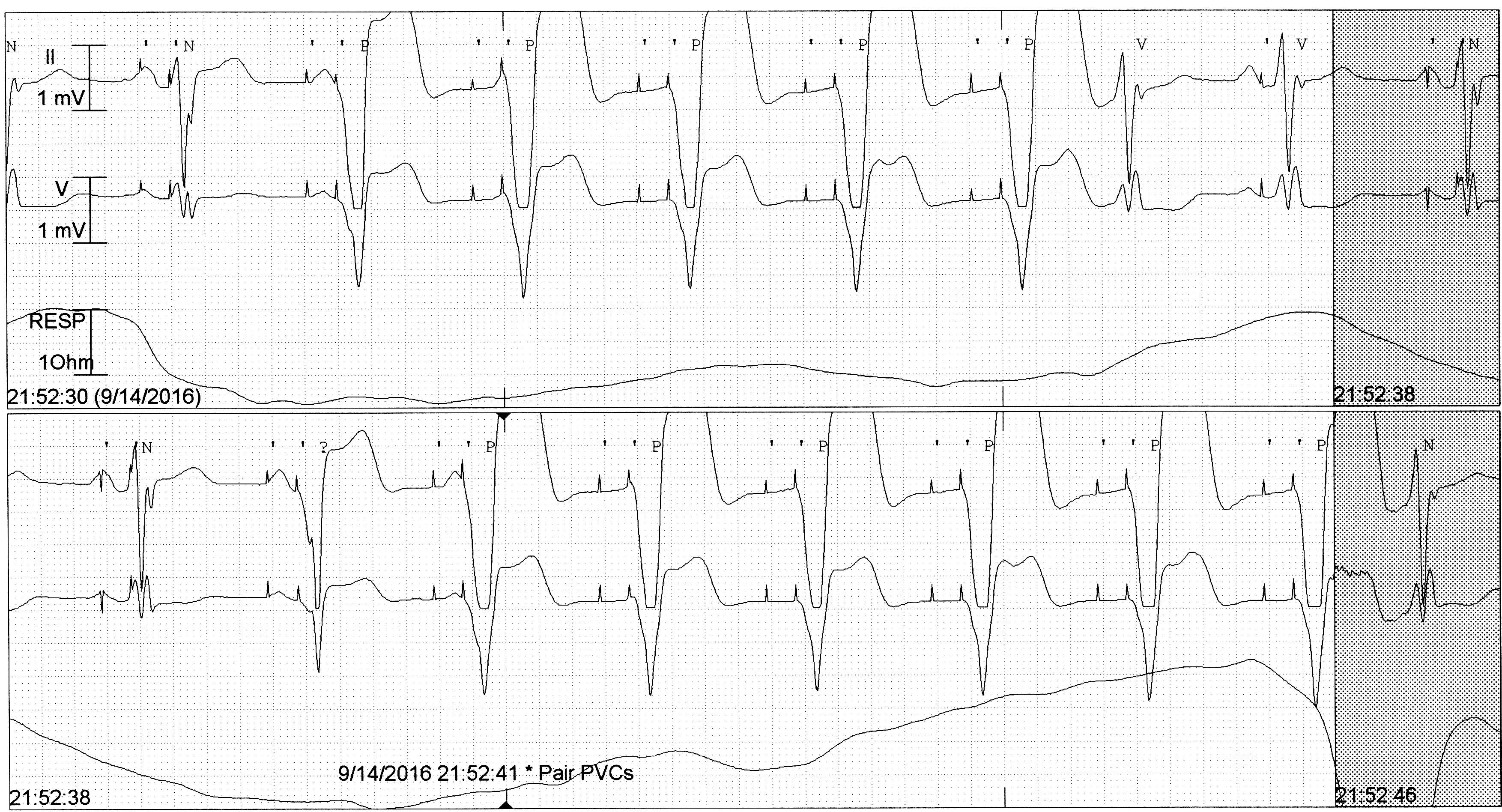 3
3
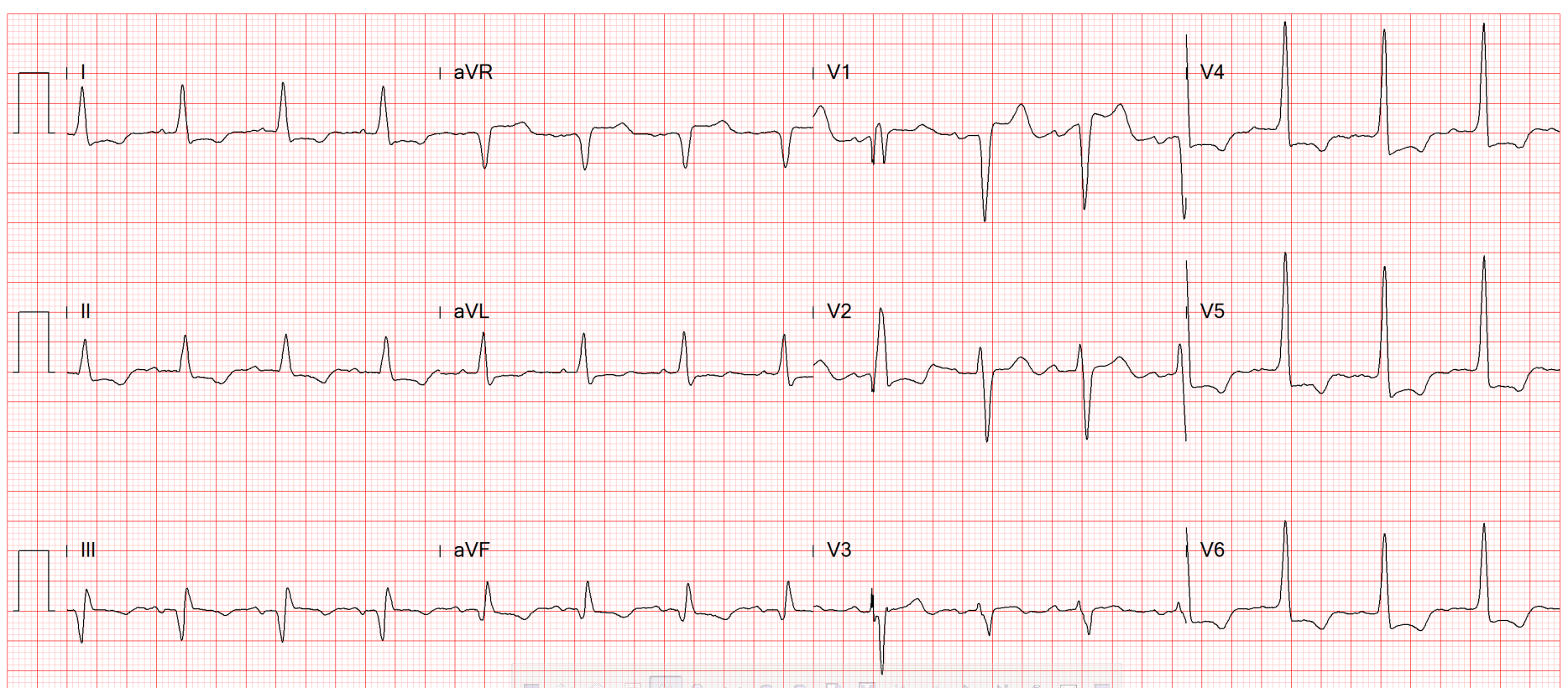 4
4
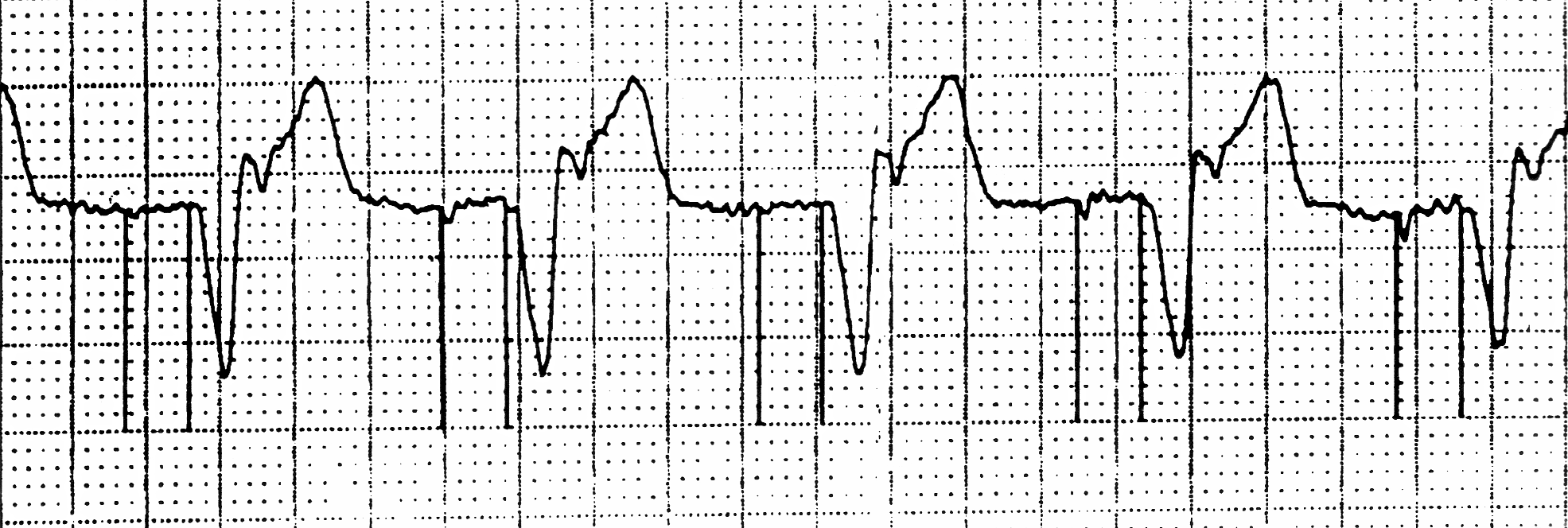 5
5
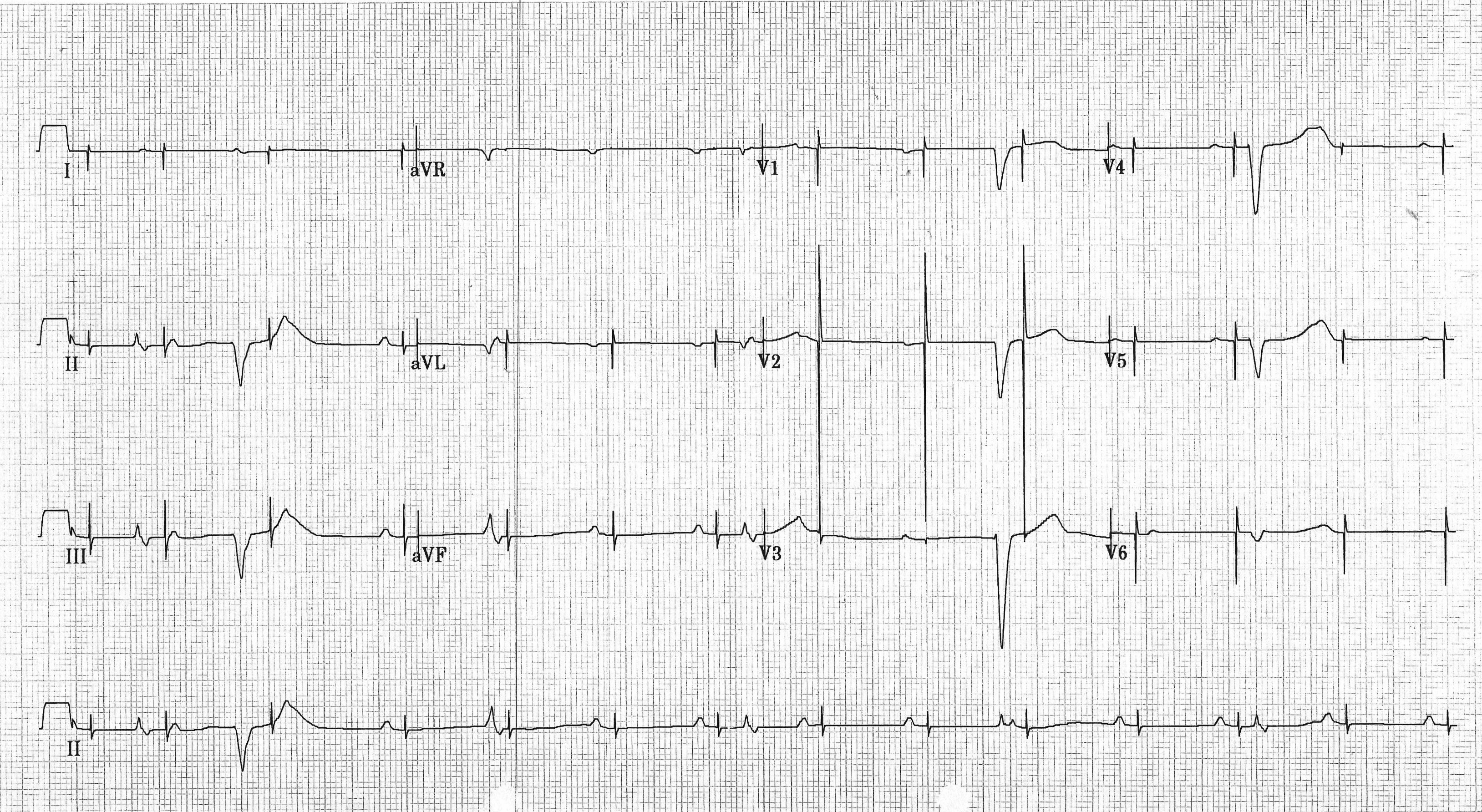 6
6
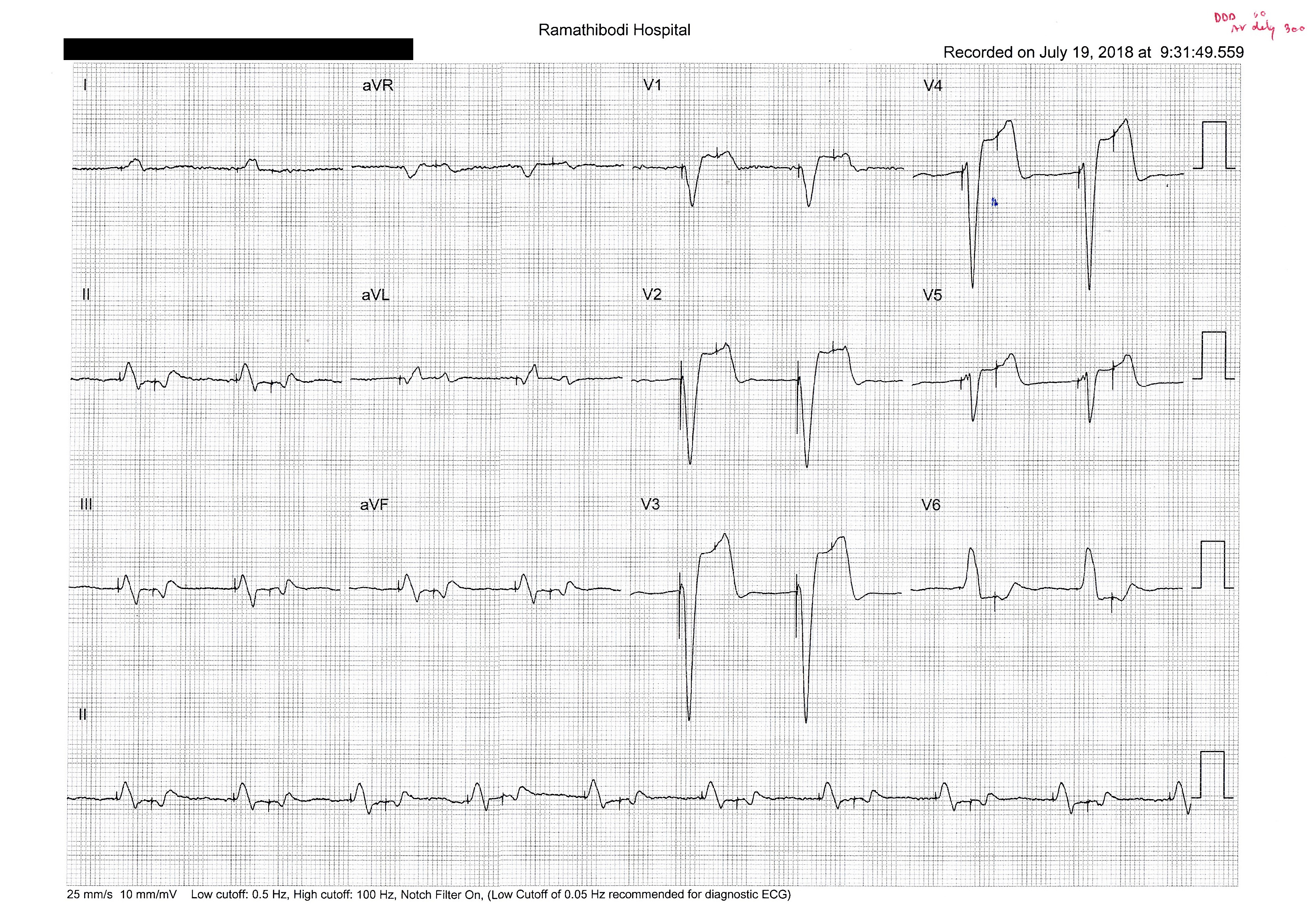 7
7
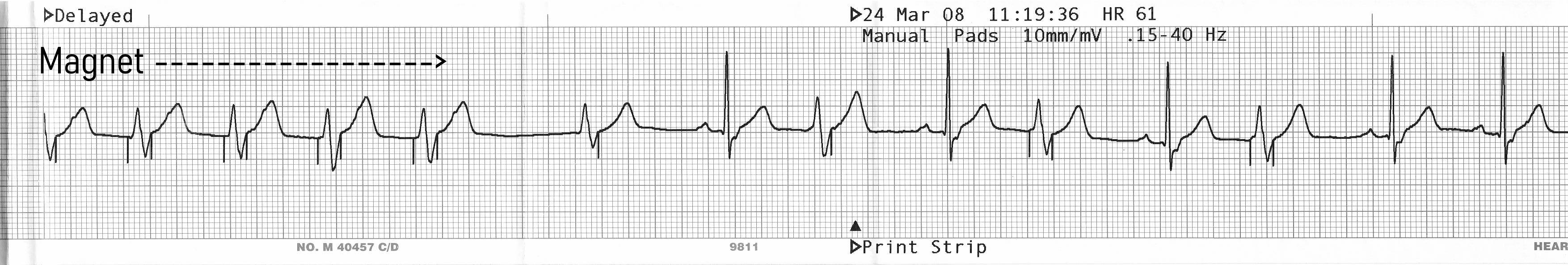 8
8
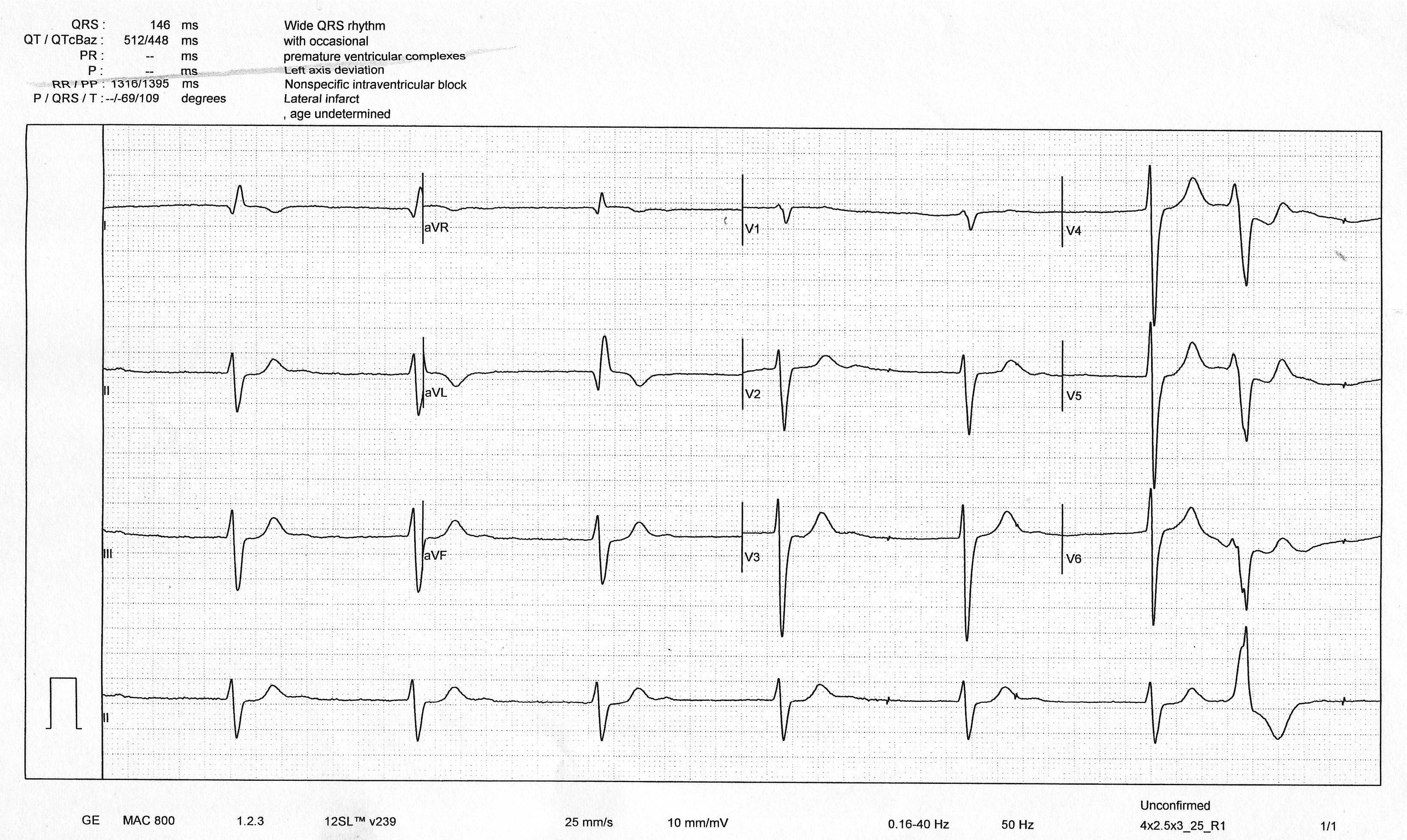 9
9
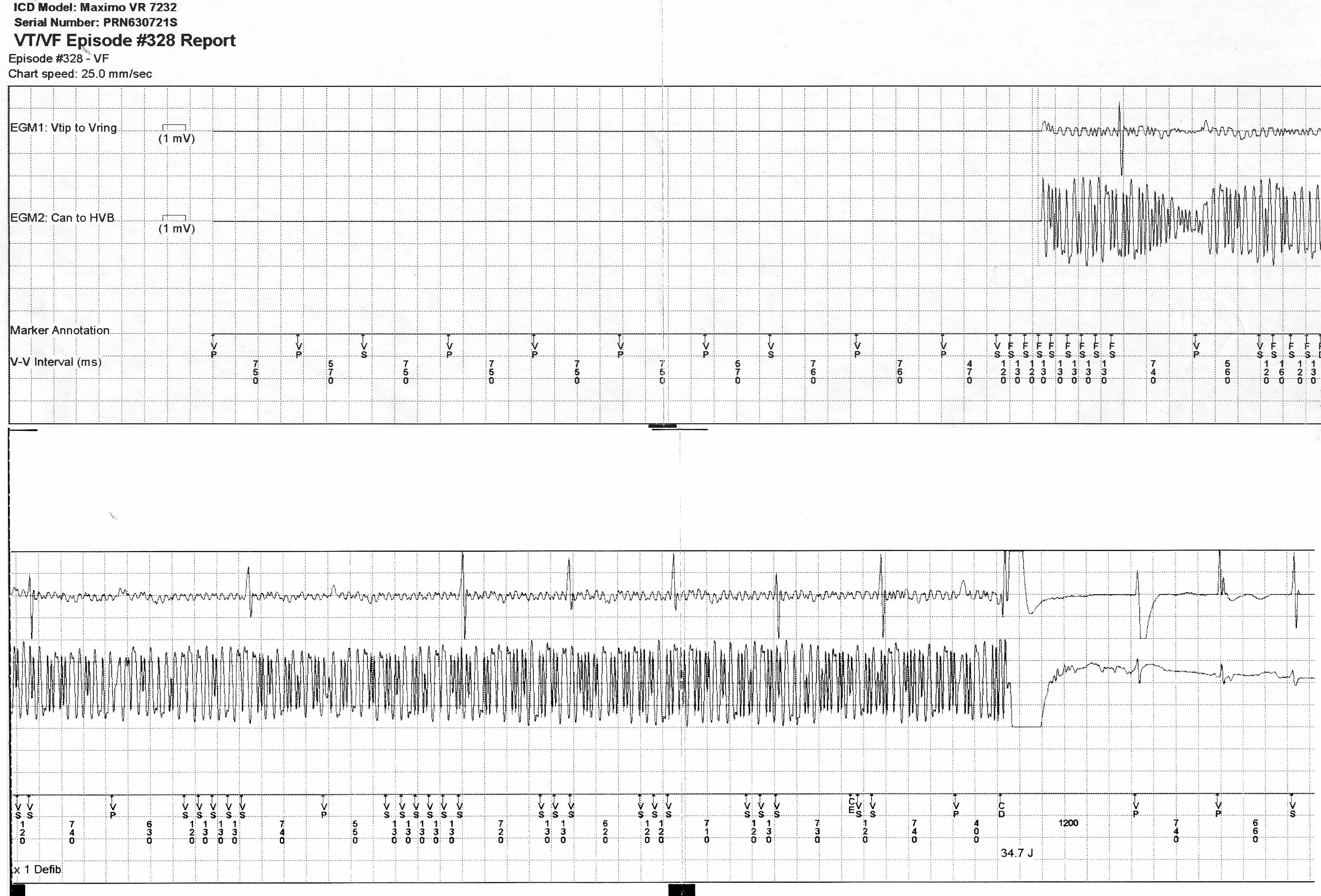 10
10
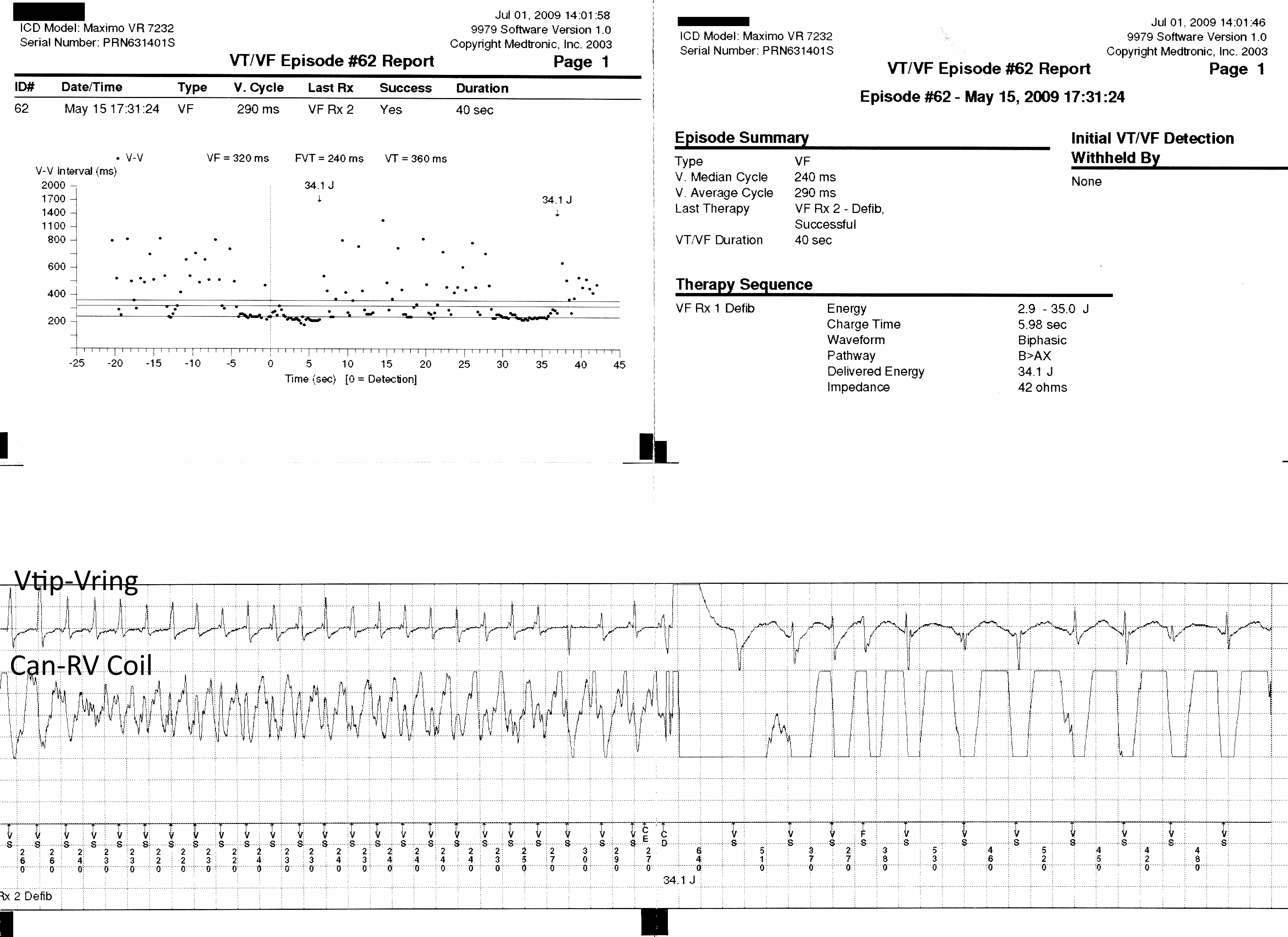 11
11
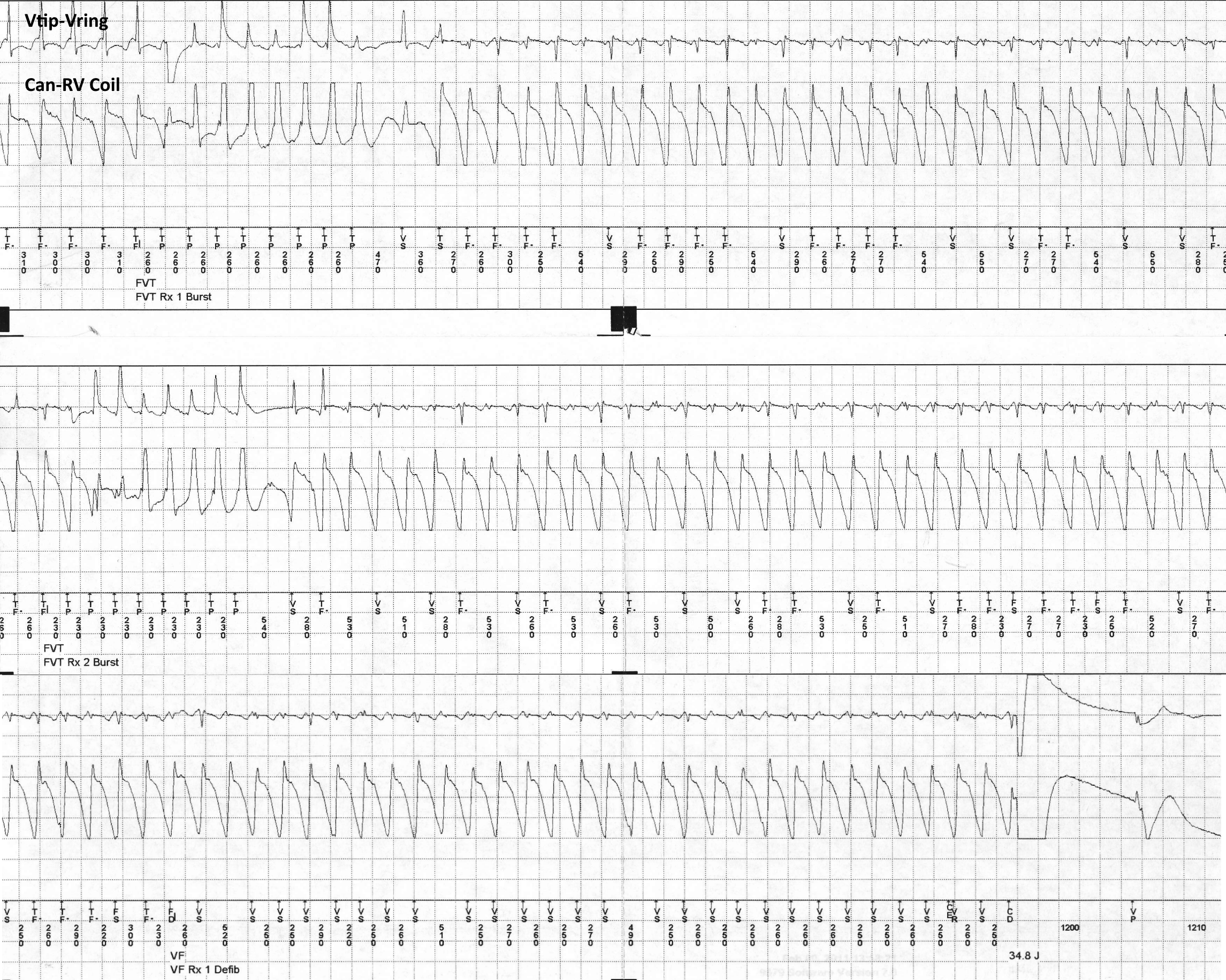 12
12
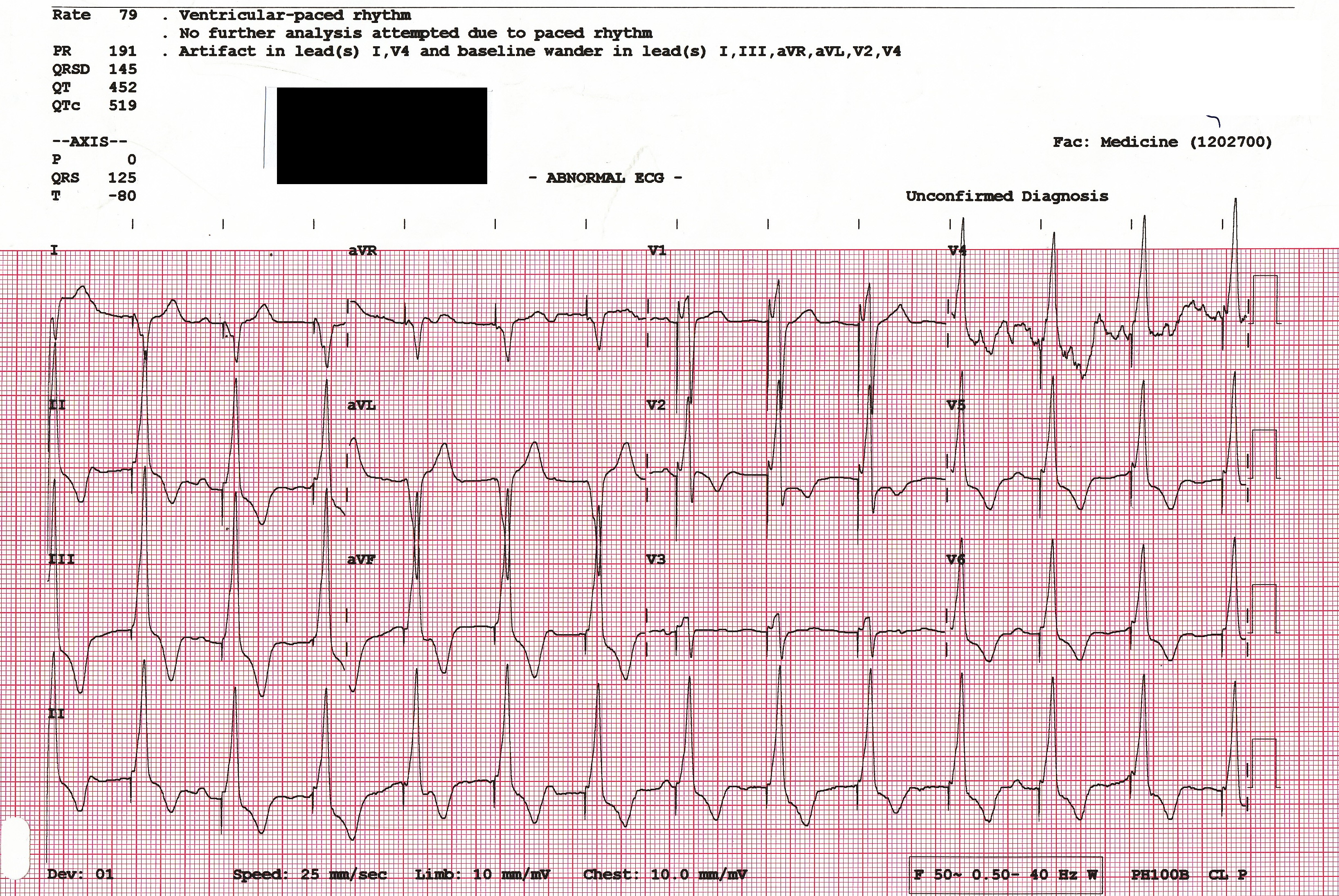 13
13
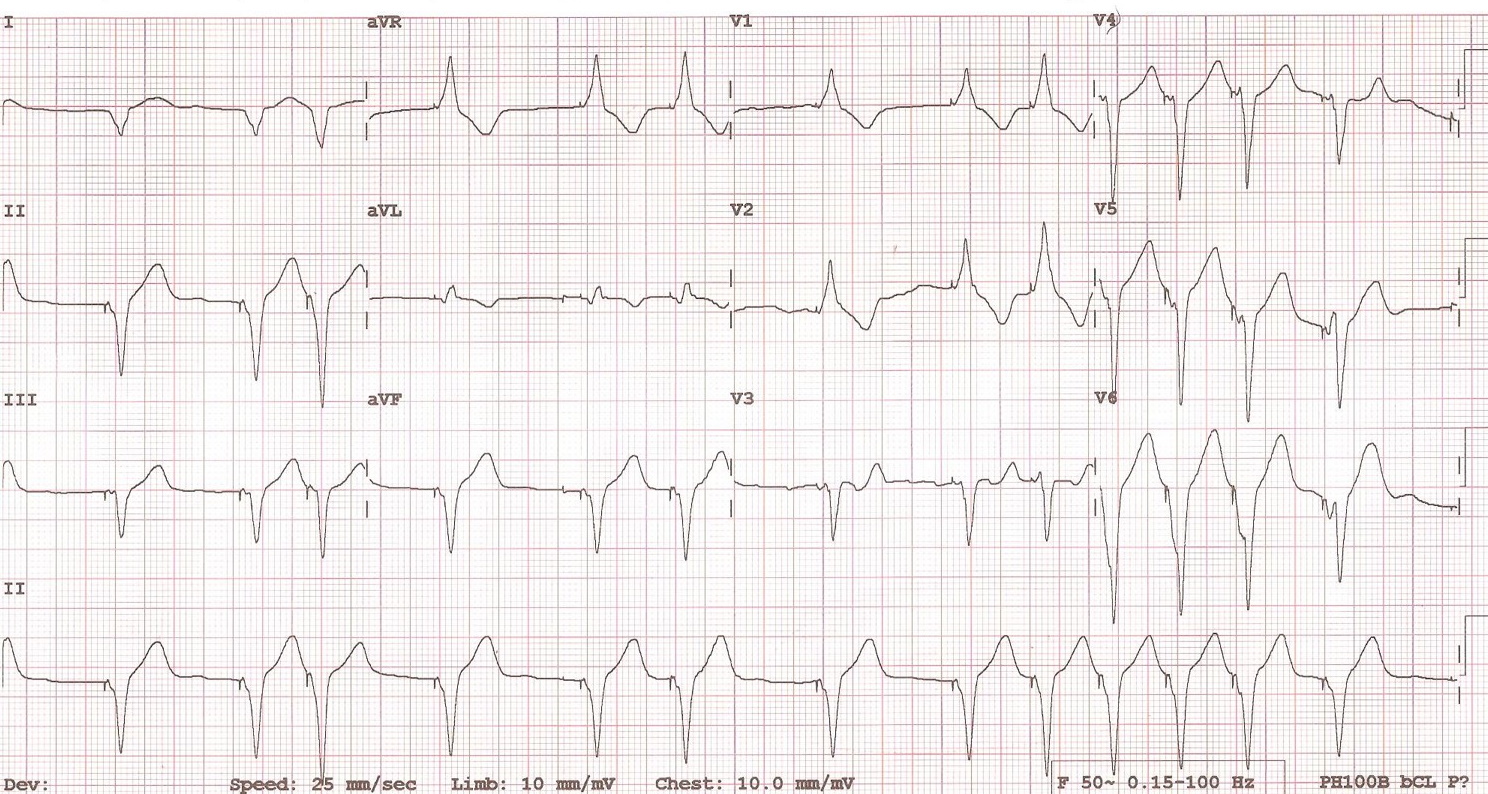 14
14
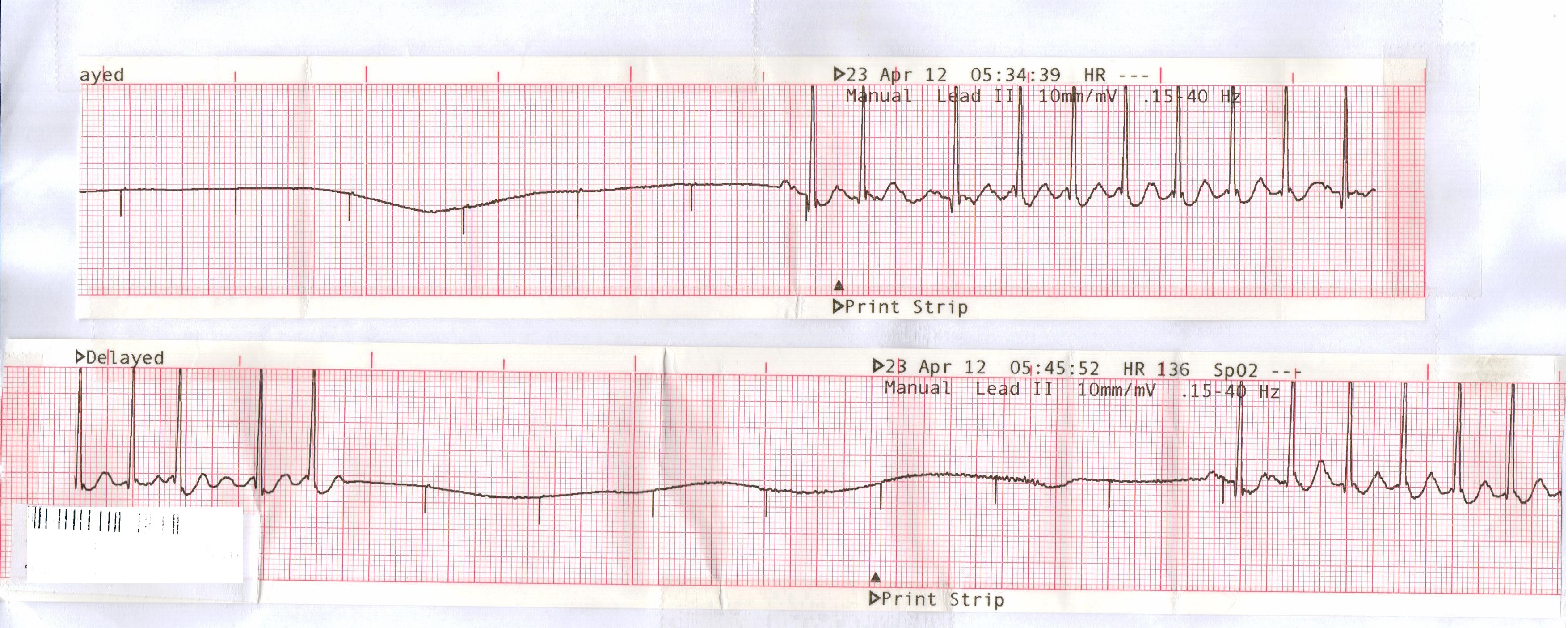 15
15
 1
1
 2
2
 3
3
 4
4
 5
5
 7
7
 8
8
 10
10
 11
11
 12
12
 13
13
 14
14
 15
15
Heart Rhythm Box is a collection of web-paged style presentations in clinical cardiac electrophysiology topics.
The page is created mainly for educational purpose.
© CODING OF A KIND
design to your style · write to your need
design to your style · write to your need